Diving deep into the world of dermatology, this article aims to shed light on common skin issues that plague many. It’s a guide that navigates through the labyrinth of skin conditions, offering essential insights to help understand them better.
From acne to eczema, psoriasis to rosacea, the skin’s tale is as diverse as it’s complex. The article ventures into these common issues, unraveling their causes, symptoms, and possible treatments.
Acne: The Common Adolescent Ailment
Acne ranks as the most prevalent skin concern among adolescents. Most know it by its signature symptoms: erupting, red pimples, blackheads, whiteheads, and nodules. These visible eruptions result from the obstruction of small pores in the skin, often due to oily secretion or dead skin cells. Teens encounter these aggravations largely due to hormonal changes during puberty. However, adults aren’t immune, with women noticing flare-ups during menstruation or pregnancy, stressing the importance of understanding acne’s complexity. While discussing potential treatments like over-the-counter products and prescription medications, it becomes apparent that a customised approach might be the most effective. Acne’s multifaceted nature, with genetics, diet, and stress playing potential roles, underscores the need for stealth and precision in tackling this common skin ailment.
Eczema: The Itchy Inflammation
Next in line is eczema, another common skin ailment that plagues many individuals. Technically termed ‘atopic dermatitis’, eczema frequently manifests as dry, itchy skin accompanied by a rash, often on the hands, feet, or face. The exact cause remains unknown, but experts suggest a combination of genetic and environmental factors. For those affected, effective childhood eczema treatment options can help manage symptoms and improve the quality of life for both children and their families.
Managing eczema involves moisturizing the skin regularly, avoiding triggers that cause flare-ups, and in certain cases, medication can offer relief. Unlike acne, where location-based treatments like varicose vein removal in London do not apply, eczema’s reach is broad and solutions less location-specific, stressing the need for general awareness and effective management strategies. As a side note, experts recommend enrolling in safety training, just like first aid training in Edmonton, to learn how to treat possible complications or itchiness.
Psoriasis: The Chronic Condition
Psoriasis emerges as a chronic, recurrent skin disorder. Defining features include red patches adorned with thick, silvery scales typically located on knees, elbows, and scalp. With origins tracing back to an overactive immune system, this skin issue speeds up skin cells’ growth. While it’s not contagious, a combination of genetic factors and environmental triggers, ranging from stress to weather changes, influence its development.

Treatment options balance on a spectrum from topical creams to ultraviolet light therapy. In specific cases, doctors might recommend systemic treatment, incorporating oral or injectable medicines, when other treatments don’t alleviate symptoms. Regrettably, psoriasis has no known cure, but its disruptive impacts can be managed using established and effective strategies. Comparatively, the multifaceted nature of skin disorders like acne or the generalized approach required for conditions like eczema, managing psoriasis calls for a carefully tailored strategy. The focus is on reducing the rapid growth of skin cells and soothing discomfort. Over time, affected individuals may notice an ebb and flow in symptom severity, highlighting the chronic and recurring nature of psoriasis.
Varicose Veins: A Vascular Concern
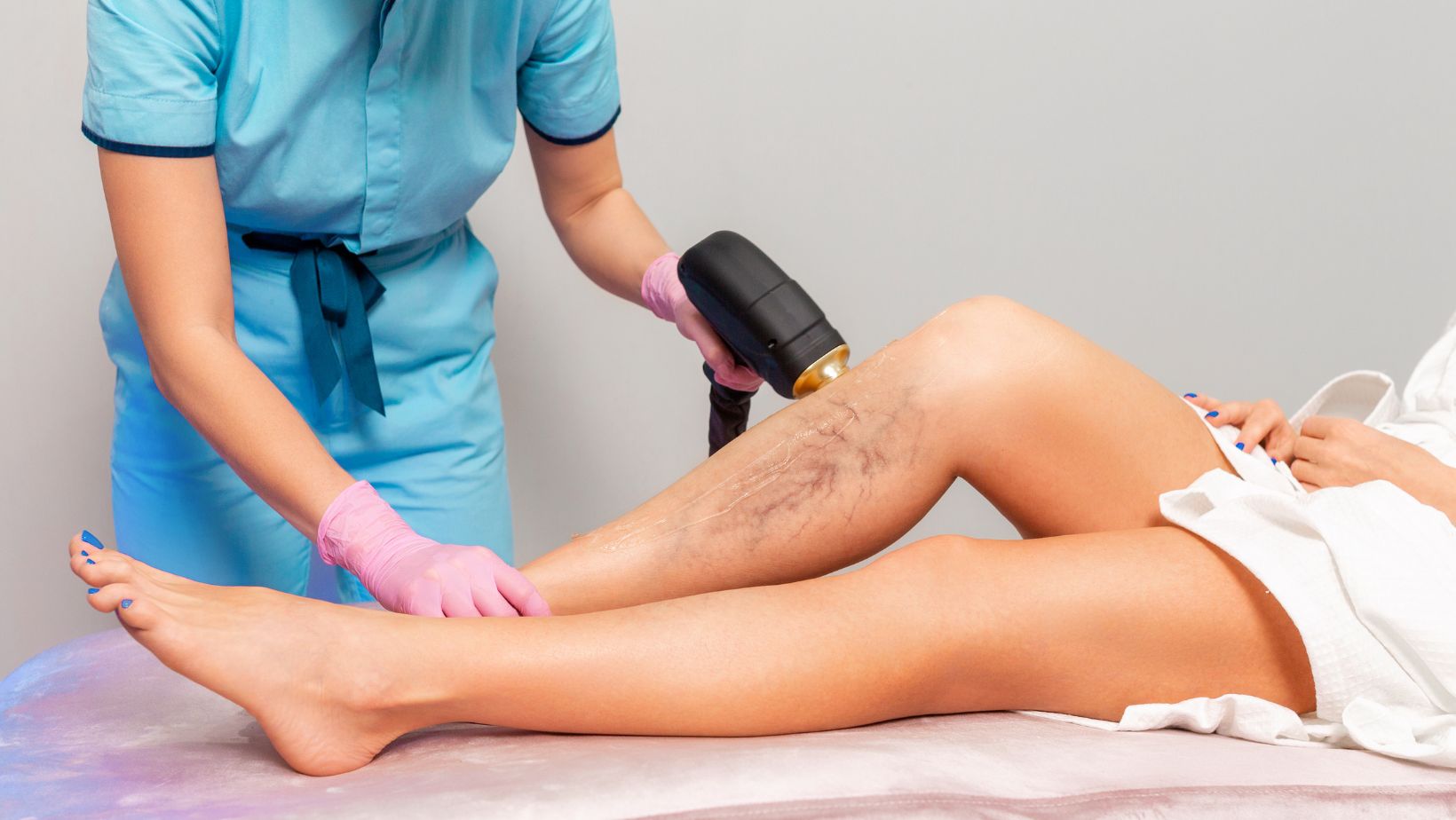
Switching gears, the discussion navigates to varicose veins, a vascular issue that often presents a unique set of challenges. Varicose veins occur when veins, usually in the legs, become enlarged, twisted, and painful, resulting from weak or damaged vein valves. The condition, unlike acne or psoriasis, isn’t localized to the skin but involves the blood vessels beneath. Management involves lifestyle adjustments, compression stockings, and surgical interventions such as varicose vein removal. In metropolitan areas, specialised clinics offer advanced treatments, and many patients seek varicose vein removal London for state-of-the-art care
Rosacea: The Redness and Blushing
Rosacea, often mistaken for acne or eczema, presents a blush or sunburn look on the skin. It’s primarily located on the face, specifically the cheeks, nose, and forehead, but can also appear on the chest, ears, and back. This chronic skin condition, unlike the vascular concern of varicose veins, typically involves persistent redness, visible blood vessels, and pink, tiny, pus-filled bumps, causing discomfort and self-consciousness in patients. Similar to managing psoriasis, or undergoing procedures like varicose vein removal in cities such as London, rosacea treatment includes various strategies. Through lifestyle modifications, appropriate skincare, and medical therapies, the severity of rosacea symptoms can be mitigated. A dermatologist often prescribes topical medications to manage inflammation but additionally may employ oral antibiotics, laser therapy, or surgical procedures in severe cases.
Rosacea’s triggers tend to be individual-specific, stressing the importance of personalized management much like the strategies followed for acne, eczema, and psoriasis. By identifying and avoiding these triggers, patients can ensure better control over their condition, fostering improved self-esteem and a higher quality of life.
Conclusion
Understanding common skin issues such as acne, eczema, rosacea, and psoriasis is just the start. It’s crucial to recognize that each condition demands a personalized approach. Psoriasis, with its chronic and recurring nature, requires tailored strategies to control rapid skin cell growth. Similarly, varicose veins, a vascular concern, isn’t merely a skin issue but involves the underlying blood vessels, necessitating lifestyle adjustments and potential surgical interventions. Rosacea, often mistaken for other skin conditions, calls for a careful identification of triggers and a combination of lifestyle modifications, skincare, and medical therapies. So, it’s not just about identifying the skin issue, but understanding its unique characteristics and managing it effectively. That’s the key to improving control over these conditions, enhancing self-esteem, and ultimately, boosting the quality of life.


















